In March 2024, a routine blood test came back with HbA1C of 6.1%, right at the border of pre-diabetes. I wasn't on any medication, but the number was a warning. Instead of ignoring it, I decided to understand my body better. What followed was 18 months of data, experimentation, and some genuinely surprising discoveries about Indian food and blood sugar.
By October 2025, my HbA1C had dropped to 5.2%, solidly in the normal range. Here is everything I did, with the actual lab reports and continuous glucose data to back it up.
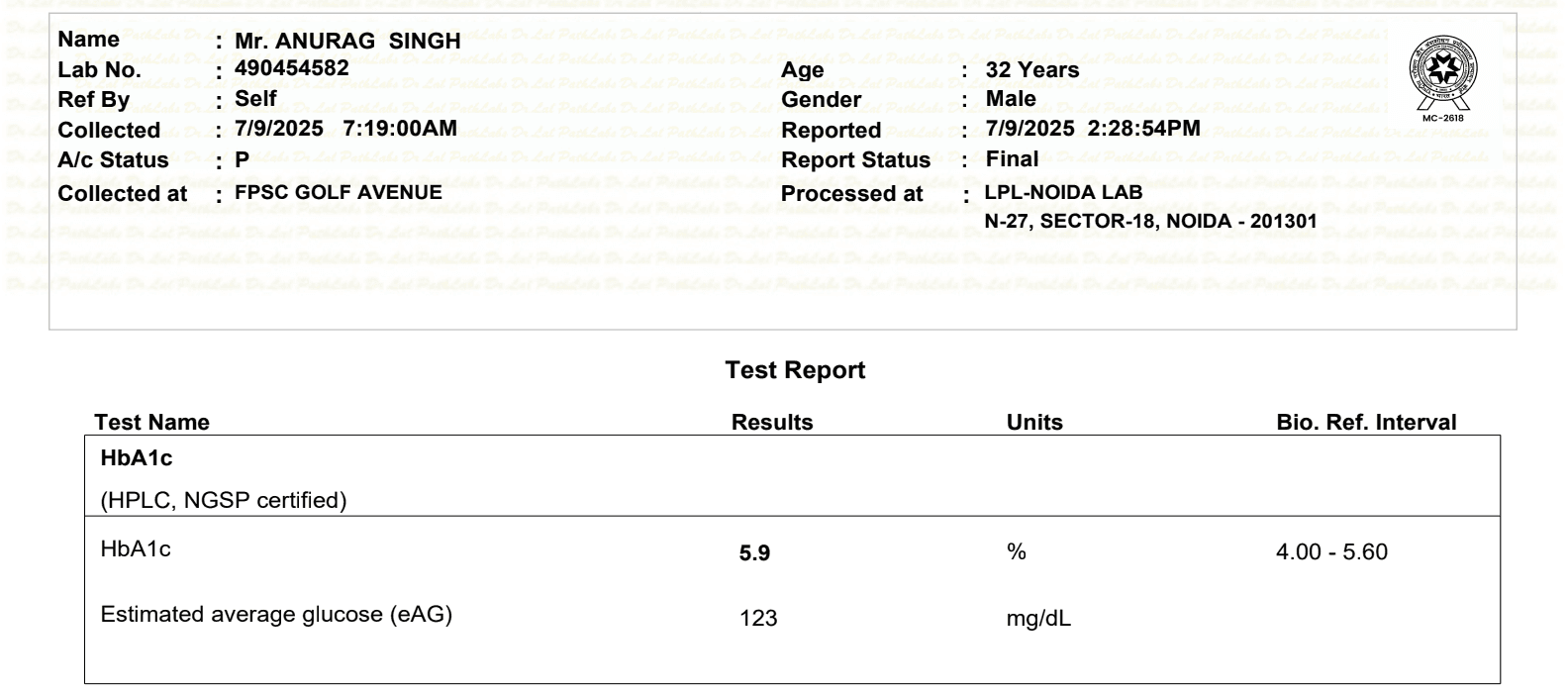
The Lab Reports
Three blood tests over ~18 months tell the whole story. Here are the actual reports:



The Tool That Changed Everything: A CGM
An HbA1C test only gives you a 3-month average. It tells you something is wrong, but not what specifically is causing it. I needed real-time data.
I bought a FreeStyle LibreSensor (a Continuous Glucose Monitor, or CGM) from PharmEasy. The sensor sticks to your upper arm and measures interstitial glucose every few minutes for 14 days. I used the Gurucose app to read the sensor and export data to CSV.
A 14-day CGM sensor that sits on your upper arm. No finger pricks. Just scan or glance at your phone to see your real-time glucose curve. The purchase receipt above is from PharmEasy, it's available at most major Indian pharmacies.
- 14 days of continuous data per sensor
- Syncs via Gurucose app (exports to CSV)
- Available without prescription
- No blood draw, reads interstitial fluid
14 Days of Real Glucose Data
Below is my continuous glucose profile across the 14-day sensor window (Jul 28 – Aug 12, 2025). Each spike is a meal. The overnight rises, especially in the first few days, clearly show the problem: my body struggled most at night.
The green band (70–140 mg/dL) is the normal fasting + post-meal range. Sustained readings above 140 after meals indicate poor glycaemic control.
Raw data from Gurucose app (FreeStyle LibreSensor). Values in mg/dL. Sampled every 5 readings for display performance.
12 Things I Learned About My Body
Two weeks of CGM data is more educational than years of guessing. Here's what the data showed me. Some expected, some genuinely surprising.
Night spikes were my biggest problem
Even eating the same meal, my glucose spiked much more at dinner than at lunch. My sedentary office work during the day seemed to blunt the lunch spike. Dinner = danger zone.
80g paneer reduced my dinner spike by ~20%
Adding a serving of paneer (cottage cheese) to my dinner meaningfully flattened the glucose curve. Protein slows gastric emptying, giving your body more time to handle carbs.
2 boiled eggs or an omelette kept glucose nearly flat
Eggs were the single most effective food change I made. With eggs in the meal, my spike stayed within 10–20% of baseline. No drama.
Wheat roti and rice cause similar spikes
I tested both carefully. Surprise: white rice and wheat roti produced nearly identical glucose responses for me. Neither was clearly 'safe'.
Multigrain roti was a disappointment
My blend was 50% wheat, 10% jowar, 20% besan, 20% ragi, and the glucose spike was almost identical to plain wheat roti. Context matters more than the flour.
Apple Cider Vinegar (ACV) does wonders
Having ACV (with or without lemon juice) before or during a meal produced a noticeably lower spike. The acetic acid slows starch digestion. This is one of the most evidence-backed food hacks.
Salad with lemon juice blunted spikes
Cucumber with lemon juice and salt before or during a meal reduced my post-meal spike. The lemon's acidity seems to slow glucose absorption. Add lemon to your meals.
Tea does spike glucose but less if you're active
2–4 cups of tea per day did cause small spikes, but they were noticeably less when I was doing something physical vs sitting still. Stay moving.
20 min post-dinner walk: didn't help much for me
Walking after dinner is commonly recommended, but in my personal CGM data it didn't make a significant difference. Your mileage may vary.
Cheese burst pizza: surprisingly low spike
The fat in the cheese slows digestion significantly. High fat meals can sometimes produce lower immediate spikes, though they can cause prolonged elevation.
Stale rice and roti from the fridge spike less
Cooling cooked carbs overnight converts some starch to resistant starch, which your body can't digest as rapidly. Leftover rice is literally healthier.
Context is everything: same food, different response
Stress, sleep quality, time of day, activity level - all of these changed how my body responded to the exact same meal. A CGM teaches you this viscerally.
My Simple Formula
Add acid to every meal
Lemon juice, ACV, or salad with lemon. This alone can reduce your spike by 20–30%. Add it to dal, raita, or as a side.
Always add a protein source
Eggs, paneer, dal, tofu - pick one. Protein slows carb absorption and keeps you fuller longer. Non-negotiable.
A small amount of fat helps
Fat slows gastric emptying. A little ghee on roti or cheese in a meal smooths the glucose curve.
Eat your rice and roti - but pair every meal with acid + protein + a little fat. That combination is what actually moved the needle for me.
How I'd Approach This for a Family Member
If someone in my family had elevated HbA1C, here's exactly what I'd do:
- 1
Buy a CGM sensor (FreeStyle LibreSensor from PharmEasy). 14 days of data is worth more than any nutrition advice.
- 2
Track their existing diet for 7 days without changing anything. Understand the baseline, which meals cause the worst spikes for them specifically.
- 3
Target the single worst meal first. Add acid (lemon/ACV) and a protein source. See if it moves the needle in the data.
- 4
Iterate one change at a time. The CGM gives you feedback in real-time. No guessing needed.
- 5
Retest HbA1C after 3 months. If it's moving in the right direction, keep going. If not, reconsider with a doctor.
Important Disclaimer
- I am not a medical professional. This is a personal account, not medical advice.
- Results are highly individual. Your body may respond differently to the same foods.
- If you are on insulin or diabetes medication, do not change your diet without consulting your doctor. Dietary changes can cause dangerous hypoglycaemia.
- Pre-diabetes is a spectrum. My case was mild (borderline). More advanced diabetes requires professional management.
- Think of this as a starting point for your own investigation, not a prescription.
Questions People Ask
Related Reading
Protein & blood sugar - the science
Want to understand why protein flattens glucose spikes? We broke down the research.
Read the Article